If you’ve avoided living under a rock, you probably already know what psoriasis is or at the very least, that it’s a condition that affects one’s skin.
In fact, it’s a very common autoimmune condition in the United States, affecting more than 7.5 million.
Psoriasis is a chronic skin condition characterized by thick scaly plaques on the elbows, knees, and scalp. While never contagious, the condition can lead to significant psychosocial stress surrounding one’s own appearance and flakiness. Some studies suggest that the impact of psoriasis on a patient’s mood can rival even terminal illness. Good news is that dermatologic care for patients afflicted by psoriasis has vastly improved over the last 5 years.
Psoriasis is an autoimmune disorder that affects a person’s skin. It tells your body to produce new skin cells in a matter of days instead of a skin cell’s normal cycle, which is about 28 days for an adult (though this slows progressively as we age).
Psoriasis typically runs in cycles, worse in the winter because of dryness and wind chapping and better in the summer because of ultraviolet light exposure, which can actually suppress a psoriatic flare. Plaques are uncomfortable, but less commonly itch.
The symptoms of psoriasis are pretty standard across the board. You can develop red patches of skin with scaly texture, dry and cracked skin that bleeds, thick or ridged nails, swollen and stiff joints, and even some itching, burning, or soreness.
There are 3 less common variants of psoriasis that serve mention because they often throw clinicians off the trail of a correct diagnosis:
Guttate psoriasis – Small “rain drop” plaque lesions are found throughout the body. Often triggered by strep throat.
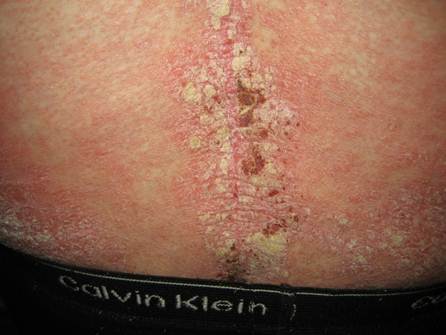
Inverse psoriasis – Inverse because these wet, red plaques affect intertriginous areas of the skin (areas that rub together like armpits, groin, and between buttocks) instead of the usual knees and elbows for which psoriasis is known.
Pustular psoriasis – Most commonly found on the hands and feet, this subtype of psoriasis appears just like it sounds…small pus-filled blisters on a red base.
Thankfully, this is not a contagious skin condition.
Unfortunately, however, little is known about the true cause of psoriasis. It is believed to be an autoimmune condition wherein your body’s T cells (the ones responsible for attacking unhealthy cells) attacks healthy ones instead, causing the symptoms.
There is much still to be learned when it comes to this skin condition and the more awareness surrounding it, the more answers we can find.
Although there is no cure for psoriasis, recent advancements in our understanding of the immunology behind this condition has led to the development of selective immuno-modulators. Unlike older immunosuppressives (like prednisone) that blunt the body’s entire immune system, these newer agents target only those arms of the immune system that are responsible for psoriatic flares.
The goal of treatment is to slow the skin cell turnover that leads to plaque formation and inflammation.
We also highly recommend UVB therapy to treat psoriasis. This works by allowing the UVB rays to penetrate the skin, which slows the growth of the psoriasis affected cells.
In order to see the best results, we recommend controlled exposure to artificial UVB light sources for a set length of time on a regular schedule. Our trained professionals can formulate the best plan for this based on your specific needs.
In addition to this advanced option, there are topical treatments, light therapy, and medications to reduce the severity of psoriasis symptoms.